
Dzulkefly and Muralli (Photo: SooPhye)
According to the World Health Organization (WHO), an estimated 604,000 new cases of cervical cancer were recorded globally in 2020. That same year, the disease claimed 342,000 lives, painting a jarring and devastating picture of the severity and lethality of the fourth most common cancer among women worldwide.
In Malaysia, cervical cancer occupies the third spot on the list. It comes after colorectal cancer, which is after breast. But unlike the two most malignant diseases out there, cervical cancer is highly preventable.
For context, the human papillomavirus, also known as HPV, is the cause in most cases of cervical cancer. Almost all sexually active people would have been infected with HPV at some point in their lives, but the immune system usually clears it from the body. However, persistent infection with high-risk HPV may cause abnormal cells to develop, which can then become cancerous.
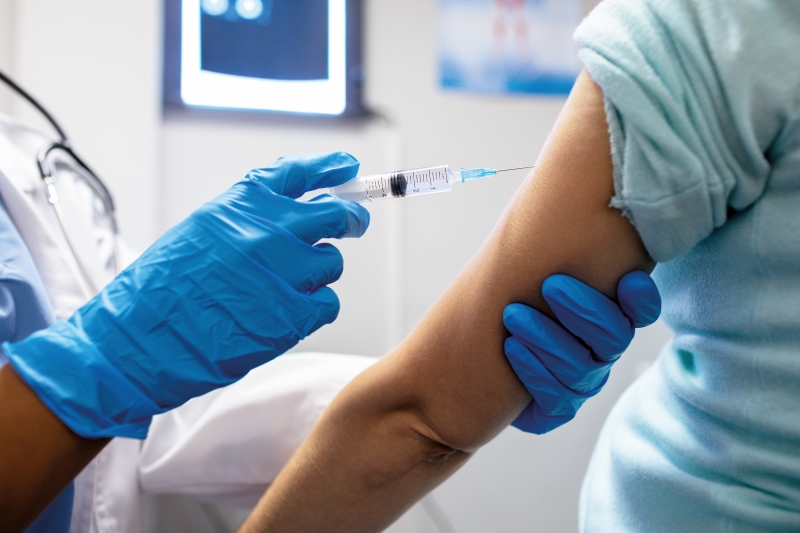
The good news is that there are HPV vaccines available for women to protect themselves against the infection with an efficacy rate that is above 90%. The bad news? Not everyone can afford it.
Prices start at around RM500 per dose and can go well into the thousands depending on the number of HPV strains it protects against as well as the fees imposed by different medical institutions. Previously, a three-dose schedule across six months was recommended, especially for older women, but new guidelines from WHO’s Strategic Advisory Group of Experts on Immunisation show that a one- or two-dose schedule is adequate and still highly effective.
In 2010, the government introduced the HPV vaccine into our National Immunisation Programme. Form 1 female students would get their jabs at school and that covered a good portion of the targeted population. However, there was still a percentage of young girls that fell out of this catchment due to disadvantaged circumstances. This is why the National Cancer Society Malaysia (NCSM) is embarking on a strong new campaign to support this underprivileged and vulnerable group.
img_5827_-_copy.jpg

Whole-of-society approach
“Leaving No One Behind: Eliminating Cervical Cancer in Malaysia” was created as a complementary programme to the existing efforts of the Ministry of Health (MoH). It is a particularly noteworthy endeavour as it is perhaps one of the foremost examples of agreement and cooperation between the government and private and non-profit bodies.
“This programme is unique because it is the first time that a ministry — particularly the Malaysian Ministry of Health — the Malaysian parliament through the Dewan Rakyat’s Parliamentary Special Select Committee (PSSC) on Health, government agencies, private industries and non-governmental organisations (NGOs) [are coming] together to run a programme that benefits the entire Malaysian community,” said Datuk Seri Dr Dzulkefly Ahmad at the campaign launch last November.
At the time, the Kuala Selangor MP and former health minister, who served during Tun Dr Mahathir Mohamad’s administration, was chairman of the PSSC on Health. A few weeks later, he was reinstated as health minister in the new cabinet line-up, replacing Dr Zaliha Mustafa, who is now in the Prime Minister’s Department (Federal Territories).
At his Putrajaya office, along with NCSM managing director Dr Murallitharan Munisamy, Dzulkefly shares that it was the NGO who first approached him about the programme.
“I must say I’m a real advocate of the ‘whole-of-society’ approach,” he starts. “Dr Muralli and NCSM came to me because they secured 300,000 doses of HPV vaccines amounting to RM90 million [donated by pharmaceutical manufacturer MSD]. And you know, being only a chair of PSSC, my main stumbling block would be how to bring an NGO into parliament and address it to the front bench.
“That was when I approached the Dewan Rakyat speaker [Tan Sri Johari Abdul] with Dr Muralli and we were so delighted that he embraced the programme very willingly. This is about the first national programme for the 15th parliamentary session, so we’re glad to be leading the objective and intention of the speaker to see how our PSSC could be leveraged and governed with the ‘whole-of-society’ approach.”
Muralli emphasised that this was not meant to duplicate existing efforts — it serves as a dovetail that will cater to the vulnerable and low-income group instead.
“The school programme is very comprehensive. All secondary schools in the country, irrespective of whether they are located in the most remote part of Sarawak or in PJ, will be part of it. When we went to Datuk Seri [Dzulkefly], the worry and concern was that it might get ‘eaten up’ by the urban programmes.”
NCSM is targeting those who are not in the school system: primary school dropouts, single mothers, teenage girls who live in extremely remote areas, working teens, those who are disabled or infirm, and imprisoned girls.
“Why Datuk Seri suggested we go through the political constituencies is because you already have that machinery interacting with the MP’s office,” Muralli explains. “They’re already serving the rakyat. They are the ones who know where the single mothers or the OKUs [Persons With Disabilities] are.”
“We have 222 if you want to count them all, and that would really mean you have a footprint in every parliamentary constituency,” Dzulkefly chimes in. “You cover the whole country. And it’s just not about MoH or NGOs; it’s the entire society. And, hopefully, one of the key responsible players would be the members of parliament and of course, by extension, members of the state assemblymen. That’s how we will get to mobilise the entire society.”
Unexpectedly, it took only about two months, from that talk with the Dewan Rakyat speaker to the official launch, for it all to come together.
“I was quite surprised we got that kind of support with no qualms,” Dzulkefly admits. “There were no glitches, we had good engagement and turnout from the MPs.
stakeholder_meeting_in_kapar.jpg

Game plan
“Leaving No One Behind” will be carried out in phases, starting with a “pilot” to acquire a general idea of each area’s acceptance rate.
“We actually have stakeholder engagement at the parliamentary constituency level, where everybody’s involved, including the ketua kampung [village chiefs], NGOs, heads of longhouses … that kind of thing. We brief them on what the programme’s going to look like and then they go back and recruit participants because they will know where our targets are,” Muralli explains.
“For example, they tell us this taman or village doesn’t understand, could you give them an educational session or something? We’ll do some community talks. And then we’ll arrange to spend maybe one or two weeks in that constituency vaccinating everyone.”
As of last December, 97 out of the 222 parliamentary constituencies had booked appointments with the process resuming after New Year’s. The time frame for implementation is about 15 months, so for the rest of 2024 until the first quarter of 2025, NCSM’s mobile clinic will engage with various communities across the country to ensure educational veracity and vaccine administration.
Path to elimination
In 2020, WHO made a global call for action to eliminate cervical cancer as a public health problem, urging all stakeholders to unite behind the bold goal. Achieving this rests on three key pillars: vaccination, screening and treatment. By 2030, 90% of girls should be fully vaccinated with the HPV vaccine by the age of 15; 70% of women should be screened using a high-performance test by the age of 35, and again by the age of 45; and 90% of women with pre-cancer should be treated while 90% of women with invasive cancer should be managed. But can Malaysia meet this 90-70-90 target?
There are a few obstacles to overcome. During the three years Covid-19 put schools out of commission, the national immunisation programme was also put on the back burner. This resulted in at least 800,000 13-year-old girls missing out on being vaccinated against HPV.
“The cohorts from those years will now be pursued by MoH,” says Dzulkefly. “One cohort would have left school by now. So they are the ones we’ve got to chase after. We have to play catch-up.”
“Vaccination in schools covers maybe about 90% of the majority of Malaysians and we’re trying to top up the remaining 10% with this programme,” Muralli adds. “If we can achieve 100%, in 20 years’ time, nobody will ever have the disease. This is the goal we are targeting.
“I think this is where the whole-of-society approach comes in strong. Academic researchers providing hands-on engagement and MoH providing good policies. We hope the corporate world and business community will also chip in by way of their CSR [corporate social responsibility] contribution. Going by that trajectory, I believe we are on track to achieve elimination of cervical cancer in Malaysia by 2030.”
But vaccination is not the only key point here. Screening is equally important to detect any abnormal cell changes that could lead to the disease. NGOs like ROSE Foundation, also a partner of this initiative, offers comprehensive screenings as well as self-sampling approaches that are less invasive. However, “screening is only as good as getting treated as soon as you’re diagnosed”, Dzulkefly adds.
When detected early, cervical cancer is curable, but a late diagnosis could be fatal.
“It is a silent cancer. We’re used to this idea that you will cough, you will have some symptoms. But the symptoms in cancer, or most cancers, are not obvious right until the end. When you start bleeding, you’re already stage three or four. So that quiet period is when you need to take action,” Muralli stresses. “Women have to go for screening, which picks up asymptomatic diseases. In Malaysia, the numbers are not so alarming, but only three women out of 10 who get cervical cancer live past five years.
“If you get diagnosed — and about 40% are diagnosed late — you actually go on palliative care. You don’t even go to curative treatment. If you’re diagnosed early, you can remove your cervix and uterus, then go for chemotherapy and radiotherapy. Such patients live long and fruitful lives. ”
The data and haunting reality frustrate both men.
124670038_l.jpg
Debunking myths
A quick glance at the Malaysian National Cancer Registry shows that a total of 3,981 cases of cervix uteri cancer were diagnosed between 2012 and 2016 compared to 4,352 cases from 2007 to 2011. There is a decreasing trend, but that does not discount the fact that a sizeable number of those who were diagnosed succumbed to the disease.
There are several unfounded concerns that lead to vaccine hesitancy.
“The biggest misconception is that cervical cancer only affects those who are sexually active,” Muralli points out.
HPV is transmitted through skin-to-skin contact, which happens most easily through intercourse but one can get infected outside of it as well.
Muralli continues: “I’m a physician. I still treat patients. HPV is a very transmissible disease, so that’s something people need to be aware of.”
Infertility and becoming sexually active sooner are also common misconceptions. In fact, getting the vaccine can actually work to protect fertility as it plays a part in preventing gynaecological problems related to the cervix. As for the latter, extensive research has shown that it does not hasten sexual debut nor increase sexual engagement. It protects young women by giving them the antibodies to fight against the potential threats of cancer. And for those concerned about injecting foreign elements into the body, the HPV vaccine has been reviewed by WHO and found to be perfectly safe.
“We’ve vaccinated more than five million women in Malaysia in almost 15 years. There has been nothing to cause alarm,” Muralli states. “In the past maybe about 10 years, we started seeing very high rates of NPC, or nasopharyngeal cancer, which may be caused by HPV.”
This cancer affects the pharynx, which is part of the throat that connects the back of the nose to the back of the mouth. “So, it’s like ‘buy one, free one’, lah. You gao tim [settle] this, and it can also help prevent NPC.”
A lesser-known fact is that HPV affects males as well.
“They can get genital warts, penile cancer and whatnot. If we could vaccinate both the sexes, then the chance of it being reduced is certainly higher. For now, we’re mainly focusing on girls, but the best approach is to have both vaccinated,” says Dzulkefly.
This is common practice for most First World countries. The duo agree it is something they ought to look into in future.
Leave no one behind
“So we come back to this thing about social justice. And the problem is, like, for upper middle-income people or someone who lives within the mainstream, you get the vaccination from a school. Those who’re able to pay for it will do so. But there are people who will never be able to get it due to their social disadvantages,” Muralli explains.
“They’re already poor, and because of that they don’t have access to the vaccine. So when they do get cervical cancer, they are financially crippled as well. And you know, it’s just a vicious circle. It’s something we must do right by.”
With the new programme, Dzulkefly says, “We’re really fulfilling that mantra of universal health coverage. This is the challenge. It’s easy to say ‘leave no one behind’, but it is a very bold dream because there are bound to be marginalised groups in our country.”
The health minister shares that he has come across a number of serious cases through friends and family.
“I’ve heard many harrowing stories of the battle against cervical cancer because it predated our national vaccination programme for schools.”
In his new term, Dzulkefly wants to focus on two critical reforms: health financing and digital health transformation.
Muralli, who is still a practising public health physician, recalls a poignant encounter with a patient, who eventually died from cervical cancer. “Somewhere close to the end, she said this: ‘If I had been born 10 years later, I wouldn’t have had this disease.’
“[Freedom from that risk] is the gift we want to give every woman.”
For more information and to donate, see here.
This article first appeared on Jan 8, 2023 in The Edge Malaysia.


