
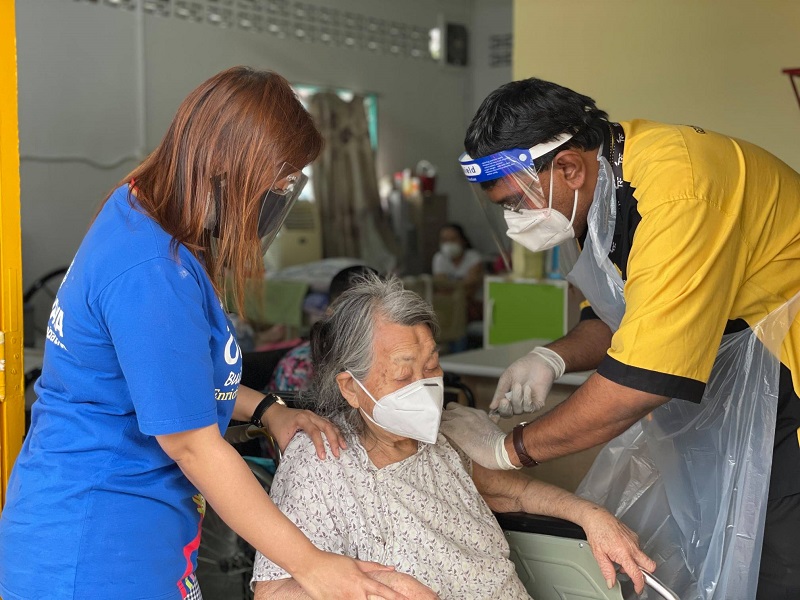
The campaign ensures that underprivileged Malaysian women are also protected from breast cancer through free mammogram screening when they get fully vaccinated for Covid-19 (All photos: National Cancer Society Malaysia)
Cancer care has been sidelined by the coronavirus, perhaps not intentionally, but for sure. People do not go for screening because they fear getting infected. Also, with hospitals full, it is not advisable to have cancer patients there because they face a higher risk of infection.
With specialists diverted to treat Covid-19 cases, radiotherapy, chemotherapy and surgery for patients have been put on hold. By the time they start seeing oncologists again, their cancer could have advanced.
“Nobody knows how bad things are on the ground. To be honest, it’s going to be about picking up the pieces for those who have not come forward with symptoms. People are suffering the impact of Covid-19 and we’re gearing up to turun padang (go to the ground),” says Dr Murallitharan Munisamy, managing director of the National Cancer Society Malaysia (NCSM).
Starting at ground zero, NCSM teams have been going from house to house since June to vaccinate cancer patients unable to leave home, the disabled and those not eligible for government welfare. “It’s very intensive and very slow — one mobile team can cover 10 to 12 houses a day — but this is the last mile. We cannot see a way back out for cancer until things return to normal. Vaccination is the only thing that can speed up people’s return to hospitals for screening and diagnoses.”
dr_murallitharan_3.jpg

About 6,000 people in the Klang Valley, Pahang, Perak, Penang and Kedah have received their jabs, with volunteers playing a big part in the programme. The Rotary Club of Damansara-West, for one, has sent drivers and cars out every weekend to take doctors and nurses around. The teams are in Johor now.
For Breast Cancer Awareness month, NCSM is seizing the chance to approach women already at hospitals for their second dose of vaccination to offer them a free mammogram scan. The Alang-Alang (Since You Are Here) campaign is for those 40 and above, with a household income of RM5,000 and below, and will run until December in 10 hospitals across Malaysia.
New Norm, Same Cancer, another initiative, will see the society working with more than 30 hospitals over the next six months to push for screening of breast, lung and prostate cancer. And, targeting men’s health, Movember, focused on prostate screening, will be held in small communities nationwide in November.
Muralli says the biggest challenge in Malaysia is not the incidence of cancer but that more than 60% of cases are diagnosed in the late stages. “That’s what we want to change.” Another problem is follow-up: “In the smaller centres, 30% of patients drop out halfway during treatment. They go and find a bomoh or alternative medicines and come back to the hospital at stage 4.”
In this pandemic, NCSM has taken the load off government hospitals by doing diagnostics. It has navigated patients whose appointments have been cancelled to clinics elsewhere, even arranging transport for them, so that their treatment will not be disrupted.
ncsm_vaccination_programme.jpg
Problem-solving is part of the social and psychological support patients get. In Hospital Melaka, for example, no cancer patient starts treatment without first meeting a society representative at least once. The office there becomes a nursery where women leave young children with volunteers when they go for chemo. At Hospital Selayang and Hospital Kuala Lumpur (HKL), staff sit with patients after they have been diagnosed to ask, “What do you need?”
With people losing their jobs and insurance coverage in turn, many cannot afford treatment in private hospitals. “Since Covid started, we’ve actively begun buying drugs as well. We negotiate directly with pharmaceutical companies to reduce prices so patients can get them cheaper. We partner hospitals to bring down the costs of procedures, such as PET scans, to offset delays in getting treatment.”
On the ground, NCSM works with hospitals to fix appointments such that women will not have to take leave and lose a day’s salary as well, or arrange for volunteers to babysit kids of single mothers when they go for chemo. Subsequently, it follows up to make sure those with symptoms are being treated.
Running services that help fill the huge gaps in government care for cancer patients is routine at NCSM, founded in 1966 by the late Datuk Dr S K Dharmalingam, Malaysia’s first oncologist. Muralli, a public health physician who also trained in health systems, last served with the World Health Organization in multiple countries before returning home in December 2017 to join the society, where he also wears the clinician’s coat.
NCSM, based behind HKL since the mid-1950s, supports itself by providing clinical services and doing projects with large corporations and international organisations. A third income stream is donations.
A good relationship with corporations helps boost funding. One successful programme coming up to four years sees Etiqa paying for 6,000 women from B40 households to have mammograms every year across 14 states. The insurance and takaful business is also behind the Alang-Alang campaign.
But Covid-19 has shrunk the society’s funds and workforce: It let go of 20% of its staff and many of the 60 left on the payroll are taking a pay cut. What has stayed strong is a volunteer force of close to 800 that does whatever needs doing.
Yearly expenditure is about RM10 million. “Last year, we were short of RM700,000. This year, so far, it’s RM500,000.” But the board is committed to continuing with its services, education, care and support. We will get by.”
NCSM reaches out to smaller communities through awareness and health programmes to help people reduce their risk of getting cancer, advocates policy, organises talks and discussions and does research on cancers and intervention. With the exception of screening, the cost of which it subsidises, all its services are free and available to everyone.
As HKL handles almost 80% of cancer treatment for children, poor patients from outstation require accommodation. The society has Children’s Home of Hope, where families can stay for as long as they need, and provides dry foodstuff and vegetables for cooking, all at no charge.
counselling_services_1.jpg

It offers wellness programmes and workshops and job training to help patients get back on track. In April 2020, it moved its mental health service online so people could call in to schedule video counselling with a psychologist. Alternatively, they can meet one face to face in seven states.
NCSM runs clinics in KL, Melaka, Penang, Ipoh, Johor and Sarawak. It is opening up services in Terengganu and trying to expand to Sabah.
Looking ahead, Muralli wants to take the society’s activities beyond the Klang Valley and make its educational materials, for laymen and healthcare professionals, available in Malay, Mandarin and Tamil too.
“Our direction has always been to go wider and deeper — expand to more places in Malaysia and do more for other communities, not just the English-speaking crowd. No one is telling the old aunties in Batang Kali anything. Without materials to influence them to change, we will just be handing out pamphlets.” Translation is a daunting task but, as always, volunteers have come forward.
After 60 years of working very quietly, NCSM is “slightly better known”, Muralli thinks. “Patients and the medical community know us. We do a lot of research and put up the papers. Our Facebook page has gently grown in the last three, four years — we have 49,000 followers compared with 6,000 before. We are doing much better in terms of gaining traction.”
This article first appeared on Oct 4, 2021 in The Edge Malaysia.


